A Cord Blood Transplant is an advanced medical procedure that uses stem cells collected from the umbilical cord blood of a newborn baby to treat various life-threatening diseases. These stem cells have the unique ability to regenerate and form healthy blood cells, making them a powerful treatment option in modern hematology and oncology.
In today’s medical landscape, Cord Blood Transplant plays a crucial role in treating cancers such as leukemia, lymphomas, and a wide range of genetic and blood disorders. It has become an important alternative when a matched bone marrow donor is not available.
Stem cells are the foundation of this treatment. They are immature cells capable of developing into red blood cells, white blood cells, and platelets. Their regenerative ability is what makes stem cell transplantation a life-saving therapy in modern medicine.
What is Umbilical Cord Blood?
Umbilical cord blood is the blood collected from the placenta and umbilical cord after the birth of a baby. Traditionally discarded as medical waste, it is now recognized as a rich source of hematopoietic stem cells. These stem cells are responsible for forming all types of blood cells in the human body. Because of their high regenerative potential, cord blood is widely used in Cord Blood Transplant procedures. After collection, the cord blood is processed and stored using a method called cryopreservation, where it is frozen at extremely low temperatures. This ensures that stem cells remain viable for years and can be used whenever needed.
How Cord Blood Transplant Works
The process of Cord Blood Transplant is scientifically structured and clinically precise:
- First, the patient receives healthy stem cells through an intravenous infusion. This procedure is similar to a blood transfusion and does not involve any surgical intervention.
- Once infused, the stem cells travel through the bloodstream and naturally migrate to the bone marrow. The bone marrow serves as the body’s primary site of blood cell production.
- After reaching the bone marrow, the stem cells begin a process called engraftment, where they start producing new and healthy blood cells. This helps rebuild the patient’s immune system and restores normal blood function.
Who Needs a Cord Blood Transplant?
A Cord Blood Transplant is recommended for patients suffering from serious and life-threatening conditions, including:
- Blood cancers such as leukemia and lymphoma
- Bone marrow failure disorders like aplastic anemia
- Genetic disorders such as thalassemia and sickle cell disease.
- Immune system deficiencies
- Certain metabolic disorders
Hospitals like Kannappa Memorial Hospital and other advanced transplant centers evaluate patients carefully before recommending this treatment to ensure safety and effectiveness.
Types of Stem Cell Transplants
Stem cell transplantation (also called hematopoietic stem cell transplantation) is used to replace damaged or diseased bone marrow with healthy stem cells. There are three main types:
1. Autologous Transplant
An autologous transplant is a stem cell transplant using the patient’s own stem cells. They are collected before treatment, stored, and returned after chemotherapy or radiation to restore blood cell production. It has very low risk of immune rejection.
2. Allogeneic Transplant
An allogeneic transplant is a stem cell transplant where a patient receives stem cells from a genetically matched donor, such as a sibling or registry match.These cells replace damaged bone marrow but may trigger immune rejection or graft-versus-host disease.
3. Cord Blood Transplant
A cord blood transplant uses stem cells collected from umbilical cord blood after birth. These cells are stored in banks and used when needed. They require less strict matching, are quickly available, but contain fewer cells, limiting use in adults.
Advantages of Cord Blood Transplant
Cord blood offers several important advantages in modern medicine:
- Less strict donor matching requirements, increasing availability
- Lower risk of graft-versus-host disease (GVHD) compared to bone marrow transplantation.
- Quick availability, as cord blood units are stored in advance
- Safer for children, especially in pediatric blood disorders
- Reduced risk of transmitting infections due to controlled collection and storage
These advantages make Cord Blood Transplant a preferred option in many complex clinical cases.
Limitations and Challenges
Despite its benefits, Cord Blood Transplant also has limitations:
- A single cord blood unit contains a limited number of stem cells.
- Slower engraftment compared to bone marrow or peripheral blood stem cells
- In some cases, two cord blood units may be required for adults
- Higher cost of storage and processing in private banking systems
These challenges are continuously being addressed through ongoing medical research.
Step-by-Step Procedure
- Pre-Transplant Evaluation: In the pre-transplant evaluation, doctors assess the patient’s health using blood tests, scans, and HLA matching tests. This helps confirm suitability for transplant and identify a compatible donor. The medical team also reviews medical history to plan safe and effective treatment.
- Conditioning Therapy: The patient is given strong chemotherapy or sometimes radiation therapy. This destroys the diseased bone marrow and weakens the immune system so the body can accept new stem cells. It also creates space in the bone marrow for new cells to grow.
- Stem Cell Infusion: During stem cell infusion, healthy cord blood stem cells are delivered into the patient through a vein, similar to a blood transfusion. The procedure is simple, painless, and does not require surgery. The infused cells then begin circulating in the body.
- Engraftment Phase: During engraftment, the transplanted stem cells reach the bone marrow and begin multiplying. They start producing new red blood cells, white blood cells, and platelets. This process is critical for rebuilding the patient’s blood and immune system and usually takes a few weeks.
- Recovery & Monitoring: After transplantation, the patient is closely monitored in the hospital. Doctors do regular blood tests, treat side effects, and give medicines to prevent infections. Continuous follow-up is needed to ensure proper healing, recovery of blood cells, and stable immune system function.
Risks and Complications
Like any major medical procedure, Cord Blood Transplant carries potential risks:
- Infections due to weakened immunity
- Delayed engraftment of stem cells
- Graft-versus-host disease (less common in cord blood)
- Organ stress due to conditioning therapy
- Bleeding or clotting complications
However,with advancedcareinspecializedcenters such as Kannappa Memorial Hospital, these risks are carefully managed.
Pre- and Post-Transplant Care
Before Transplant:
- Full medical evaluation
- Psychological preparation of patient and family
- Infection screening and preventive measures
- Lifestyle and nutritional guidance
After Transplant:
- Strict infection control and protective isolation
- Regular blood tests and monitoring
- Immunosuppressive and supportive medications
- Long-term follow-up for immune recovery
Proper care significantly improves the success rate of Cord Blood Transplant procedures.
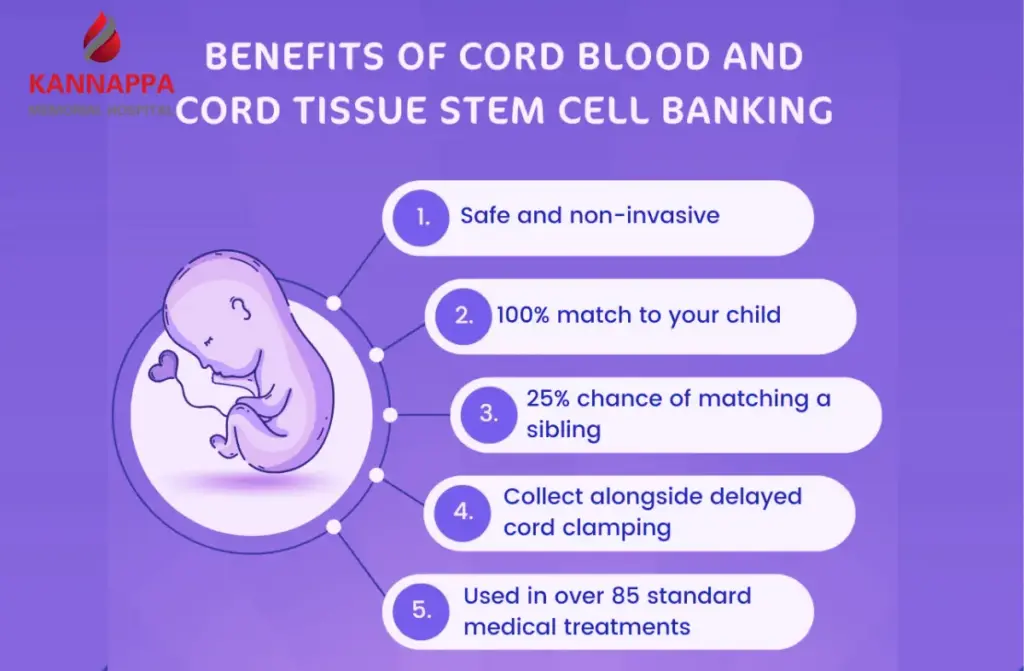
Cord Blood Banking
Cord blood banking is the process of collecting the blood left in the umbilical cord and placenta after birth, then processing and storing it in a specialized facility for possible future medical use. This blood is rich in hematopoietic stem cells, which can develop into different types of blood and immune cells.
Types of cord blood banking
1. Public cord blood banking
- The cord blood is donated voluntarily.
- It is stored in public banks and made available to anyone who needs a match.
- No cost to the donor.
- Often used for transplants in unrelated patients.
2. Private cord blood banking
- The cord blood is stored for exclusive use by the child or their family.
- Requires payment for collection and long-term storage.
- May be used if a family member develops a condition where a stem cell transplant is needed.
Why it is important
Cord blood is valuable because it can be used in hematopoietic stem cell transplantation to treat certain serious conditions such as:
- Leukemia and other blood cancers
- Bone marrow failure disorders
- Some immune system diseases
- Certain metabolic disorders
Cord Blood vs Other Stem Cell Sources
Cord blood differs from bone marrow and peripheral blood stem cells in several important ways:
- It requires less stringent HLA (human leukocyte antigen) matching
- Collection is easy, painless, and poses no risk to the donor
- It is associated with a lower risk of immune-related complications such as graft-versus-host disease
- However, it contains a lower number of stem cells compared to bone marrow or peripheral blood sources
- Each stem cell source has distinct clinical advantages, and the choice of source depends on the patient’s condition, donor availability, and the urgency of treatment.
Future Scope and Research
The future of Cord Blood Transplant is highly promising. Researchers are exploring its applications beyond blood disorders into regenerative medicine.
Ongoing studies are investigating its use in:
- Neurological disorders
- Diabetes treatment
- Heart tissue regeneration
- Autoimmune diseases
With advancements in stem cell technology, cord blood may become a key tool in personalized medicine and regenerative therapies.
Conclusion
Cord Blood Transplant is a groundbreaking advancement in modern medical science that has transformed the treatment of many life-threatening diseases. Its ability to regenerate healthy blood cells makes it a vital option when traditional bone marrow donors are not available.
With increasing awareness, improved storage techniques, and advanced treatment facilities in hospitals like Kannappa Memorial Hospital, the success rate and accessibility of this therapy continue to improve.
As research progresses, Cord Blood Transplant is expected to play an even greater role in regenerative medicine and future disease management, offering hope to patients worldwide.