Cervical cancer is a malignant disease that develops in the cells of the cervix, the lower part of the uterus that connects to the vagina. It occurs when normal cervical cells undergo abnormal changes and begin to multiply uncontrollably. The disease usually develops slowly over several years, often beginning as precancerous changes called cervical intraepithelial neoplasia (CIN). Nearly all cases are linked to persistent infection with high-risk human papillomavirus (HPV), although most HPV infections are cleared naturally by the immune system. Because it progresses gradually, cervical cancer is highly preventable and treatable when detected early, making regular screening and awareness very important.
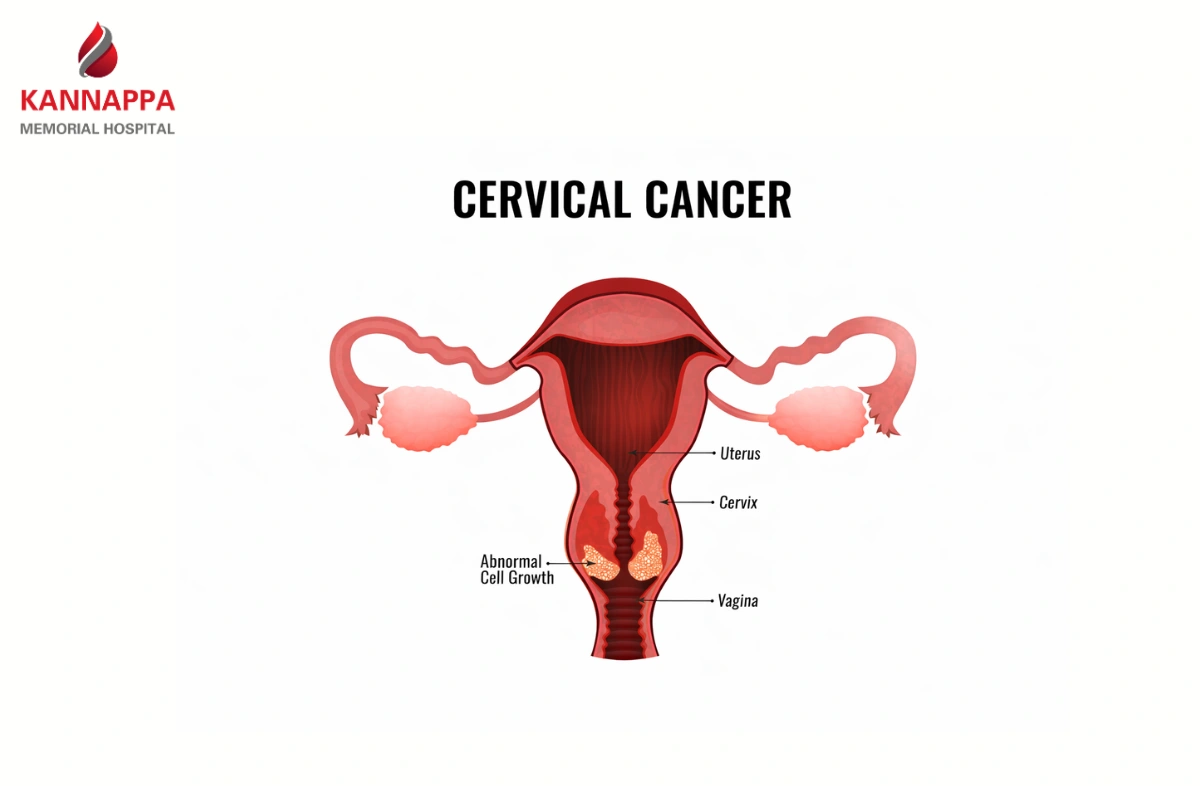
The cervix is the narrow lower portion of the uterus that opens into the vagina. It plays a vital role in reproduction, childbirth, and menstrual flow.
It consists of two main epithelial regions:
Between these two regions lies the transformation zone, which is the most vulnerable area for abnormal cellular changes. This zone is the primary site where Cervical Cancer originates, due to active cell turnover and susceptibility to HPV infection.
Understanding this anatomical region is crucial for Pap smear sampling and early detection strategies.
Cervical cancer develops due to several risk factors that increase the likelihood of persistent HPV infection and abnormal cell changes in the cervix.
The development of Cervical Cancer follows a gradual multi-step process:
If untreated, cancer can spread locally to surrounding tissues and later metastasize to distant organs.
This long pre-invasive phase is what makes Cervical Cancer one of the most preventable cancers in women.
Cervical cancer is classified based on the type of cells from which it originates. The main types differ in their location, behavior, and frequency.
Each type has different biological behavior and treatment response.
Often asymptomatic, which is why screening is essential.
Screening is one of the most effective methods for preventing cervical cancer because it helps detect abnormal changes in cervical cells at an early, treatable stage before cancer develops. Early detection greatly reduces the risk of progression and lowers mortality rates.
Regular and routine screening allows identification of precancerous conditions at an early stage, enabling timely treatment and significantly reducing the chances of developing cervical cancer.
If screening results are abnormal, further diagnostic steps include:
Imaging for staging and spread:
A multidisciplinary diagnostic approach ensures accurate staging and treatment planning.
In many tertiary care centers such as Kannappa Hospital Memorial, advanced diagnostic facilities are used to ensure early and precise detection of Cervical Cancer.
Staging of cervical cancer describes how far the disease has spread in the body. It is an important step because it helps doctors decide the most appropriate treatment and predict the outcome of the disease.
Stage I: The cancer is limited to the cervix only. It has not spread to nearby tissues or organs. This stage often has the best prognosis because the disease is detected early.
Stage II: The cancer has spread beyond the cervix to nearby tissues, but it has not reached the pelvic wall or the lower part of the vagina. At this stage, the disease is more advanced but still considered potentially curable.
Stage III: The cancer extends to the pelvic wall and/or involves nearby lymph nodes. It may also affect the lower part of the vagina and can start to interfere with kidney function due to blockage of urinary flow.
Stage IV: This is the most advanced stage. The cancer spreads to nearby organs such as the bladder or rectum (Stage IVA) or to distant organs like the lungs, liver, or bones (Stage IVB). Treatment at this stage is mainly focused on control of symptoms and improving quality of life.
Accurate staging is essential for choosing the right treatment plan and improving patient outcomes.
Treatment depends on the stage of the disease and the patient’s overall condition.
Modern oncology focuses on individualized treatment plans to improve both survival and quality of life.
Prevention is the most effective strategy against Cervical Cancer.
Vaccination programs combined with screening have significantly reduced incidence in many countries.
The prognosis of Cervical Cancer depends largely on the stage at diagnosis:
Early detection remains the most important determinant of survival outcomes.
Cervical Cancer is:
Global health initiatives aim to eliminate Cervical Cancer through vaccination, screening, and treatment accessibility.
Cervical Cancer is one of the most preventable and treatable cancers when detected early. The strong association with HPV infection provides a clear pathway for prevention through vaccination and regular screening.Public awareness, early diagnosis, and timely medical intervention are essential to reducing its burden. Healthcare institutions and community-level programs play a vital role in improving outcomes.
Hospitals such as Kannappa Hospital Memorial contribute significantly by offering screening services, diagnostic accuracy, and comprehensive cancer care support.
Cervical cancer is a malignant disease that develops in the cells of the cervix, the lower part of the uterus that connects to the vagina. It occurs when normal cervical cells undergo abnormal changes and begin to multiply uncontrollably. The disease usually develops slowly over several years, often beginning as precancerous changes called cervical intraepithelial neoplasia (CIN). Nearly all cases are linked to persistent infection with high-risk human papillomavirus (HPV), although most HPV infections are cleared naturally by the immune system. Because it progresses gradually, cervical cancer is highly preventable and treatable when detected early, making regular screening and awareness very important.
Anatomy (Site of Origin)
Causes of Cervical Cancer
Risk Factors of Cervical Cancer
Pathogenesis (Disease Development)
Types of Cervical Cancer
Symptoms
Early Detection of Cervical Cancer
Diagnosis
Stages of Cervical Cancer
Treatment
Prevention
Prognosis
Epidemiology
Conclusion
The cervix is the narrow lower portion of the uterus that opens into the vagina. It plays a vital role in reproduction, childbirth, and menstrual flow.
It consists of two main epithelial regions:
Between these two regions lies the transformation zone, which is the most vulnerable area for abnormal cellular changes. This zone is the primary site where Cervical Cancer originates, due to active cell turnover and susceptibility to HPV infection.
Understanding this anatomical region is crucial for Pap smear sampling and early detection strategies.
Cervical cancer develops due to several risk factors that increase the likelihood of persistent HPV infection and abnormal cell changes in the cervix.
The development of Cervical Cancer follows a gradual multi-step process:
If untreated, cancer can spread locally to surrounding tissues and later metastasize to distant organs.
This long pre-invasive phase is what makes Cervical Cancer one of the most preventable cancers in women.
Cervical cancer is classified based on the type of cells from which it originates. The main types differ in their location, behavior, and frequency.
Each type has different biological behavior and treatment response.
Often asymptomatic, which is why screening is essential.
Screening is one of the most effective methods for preventing cervical cancer because it helps detect abnormal changes in cervical cells at an early, treatable stage before cancer develops. Early detection greatly reduces the risk of progression and lowers mortality rates.
Regular and routine screening allows identification of precancerous conditions at an early stage, enabling timely treatment and significantly reducing the chances of developing cervical cancer.
If screening results are abnormal, further diagnostic steps include:
Imaging for staging and spread:
A multidisciplinary diagnostic approach ensures accurate staging and treatment planning.
In many tertiary care centers such as Kannappa Hospital Memorial, advanced diagnostic facilities are used to ensure early and precise detection of Cervical Cancer.
Staging of cervical cancer describes how far the disease has spread in the body. It is an important step because it helps doctors decide the most appropriate treatment and predict the outcome of the disease.
Stage I: The cancer is limited to the cervix only. It has not spread to nearby tissues or organs. This stage often has the best prognosis because the disease is detected early.
Stage II: The cancer has spread beyond the cervix to nearby tissues, but it has not reached the pelvic wall or the lower part of the vagina. At this stage, the disease is more advanced but still considered potentially curable.
Stage III: The cancer extends to the pelvic wall and/or involves nearby lymph nodes. It may also affect the lower part of the vagina and can start to interfere with kidney function due to blockage of urinary flow.
Stage IV: This is the most advanced stage. The cancer spreads to nearby organs such as the bladder or rectum (Stage IVA) or to distant organs like the lungs, liver, or bones (Stage IVB). Treatment at this stage is mainly focused on control of symptoms and improving quality of life.
Accurate staging is essential for choosing the right treatment plan and improving patient outcomes.
Treatment depends on the stage of the disease and the patient’s overall condition.
Modern oncology focuses on individualized treatment plans to improve both survival and quality of life.
Prevention is the most effective strategy against Cervical Cancer.
Vaccination programs combined with screening have significantly reduced incidence in many countries.
The prognosis of Cervical Cancer depends largely on the stage at diagnosis:
Early detection remains the most important determinant of survival outcomes.
Cervical Cancer is:
Global health initiatives aim to eliminate Cervical Cancer through vaccination, screening, and treatment accessibility.
Cervical Cancer is one of the most preventable and treatable cancers when detected early. The strong association with HPV infection provides a clear pathway for prevention through vaccination and regular screening.Public awareness, early diagnosis, and timely medical intervention are essential to reducing its burden. Healthcare institutions and community-level programs play a vital role in improving outcomes.
Hospitals such as Kannappa Hospital Memorial contribute significantly by offering screening services, diagnostic accuracy, and comprehensive cancer care support.
Cervical cancer initially spreads to adjacent tissues including the vagina, uterus, and nearby pelvic structures. It commonly involves the pelvic lymph nodes at an early stage. As the disease progresses, it can metastasize to distant organs such as the lungs, liver, and bones if not detected and treated promptly properly.
Cervical cancer is not 100% curable in all cases. However, when detected early, especially at precancerous or initial stages, it is highly treatable and often curable. Advanced stages are more difficult to cure, but treatments like surgery, radiation, and chemotherapy can control the disease and improve survival outcomes significantly.
No food can completely prevent cervical cancer, but a healthy diet may lower risk. Fruits and vegetables rich in antioxidants, such as berries, carrots, and spinach, help protect cells. Foods high in vitamin C, folate, and beta-carotene support immunity. Whole grains, nuts, and seeds are beneficial. Maintaining a balanced diet supports overall health and reduces cancer risk.
Yes, many people can live a long and healthy life after cervical cancer, especially when it is diagnosed early and treated effectively. Regular follow-up care is important to monitor recovery and prevent recurrence. A healthy lifestyle, proper treatment, and early detection greatly improve survival rates and long-term outcomes, allowing many survivors to live normal, active lives.