Multiple myeloma is a cancer of plasma cells a type of white blood cell found in the bone marrow that normally produces antibodies to help your body fight infections. When these plasma cells mutate and grow uncontrollably, they crowd out healthy blood cells, produce abnormal proteins, and cause damage to the bones, kidneys, and immune system.
Early detection is a critical factor in outcomes. At Kannappa Memorial Hospital, our dedicated oncology team understands that timely diagnosis and a personalized treatment approach can extend life, improve quality of life, and in some cases, achieve long-term remission. This comprehensive guide is designed to empower patients and caregivers with accurate, up-to-date information on every aspect of multiple myeloma.
Understanding Multiple Myeloma
What Are Plasma Cells?
Plasma cells are specialized white blood cells produced in the bone marrow. Their primary role in the immune system is to manufacture antibodies proteins that identify and neutralize harmful pathogens like bacteria and viruses. In a healthy body, plasma cells are created on demand and regulated carefully.
How Multiple Myeloma Develops
In multiple myeloma, a single abnormal plasma cell undergoes genetic mutations and begins to multiply uncontrollably. These cancerous cells accumulate in the bone marrow, crowding out healthy red blood cells, white blood cells, and platelets.
As they proliferate, they produce an abnormal antibody called M protein (monoclonal protein), which serves no protective function but can accumulate in the blood and urine, damaging the kidneys and other organs.
Why Is It Called “Multiple” Myeloma?
The term “multiple” refers to the fact that tumors typically develop at multiple sites throughout the bone marrow commonly in the spine, skull, pelvis, and ribs rather than forming a single localized mass.
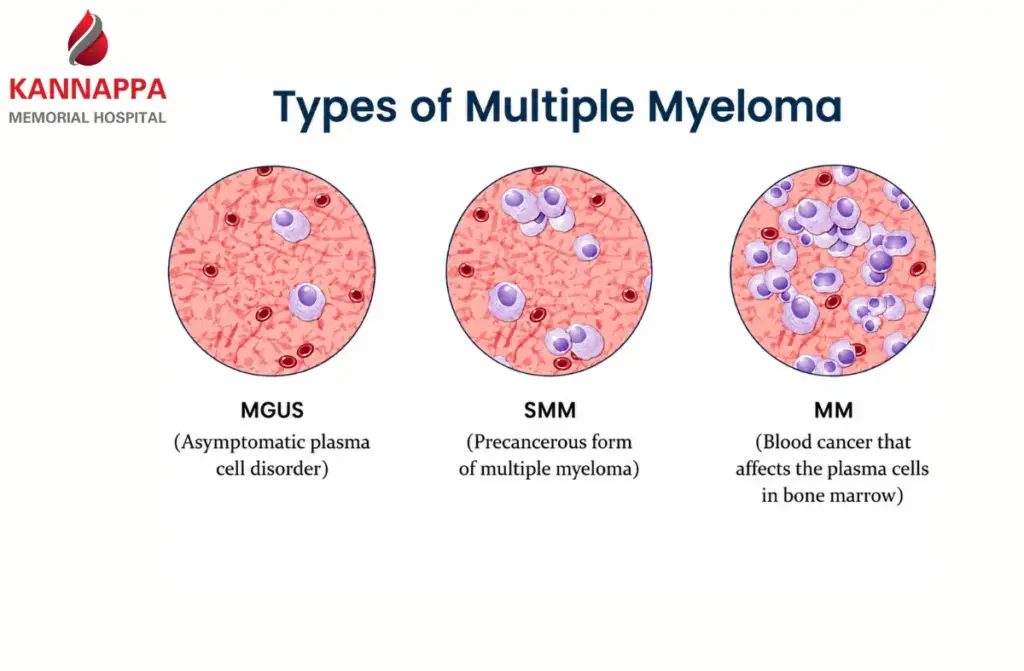
Types and Early Stages of Multiple Myeloma
Determining a patient’s position on the disease spectrum is crucial for choosing the most appropriate monitoring approach or treatment plan.
- MGUS (Monoclonal Gammopathy of Undetermined Significance): A mild, non-cancerous condition where a small amount of abnormal protein is found in the blood. It usually causes no symptoms but is monitored regularly because it can slowly progress to myeloma.
- Smoldering Multiple Myeloma: An early stage of myeloma with increased abnormal protein levels and a higher number of abnormal cells in the bone marrow, but without any symptoms or organ damage. It is carefully monitored over time to detect any signs of progression.
Active Multiple Myeloma: A full disease stage where symptoms and organ damage appear, such as bone pain, anemia, kidney problems, or infections. This stage needs treatment. - Solitary Plasmacytoma: A rare condition where a single tumor of abnormal plasma cells forms in one area of bone or tissue, without spreading throughout the body.
Symptoms of Multiple Myeloma
Multiple myeloma can be silent in its early stages. Many patients are diagnosed incidentally through routine blood tests. As the disease advances, symptoms become more pronounced.
Early symptoms may include persistent fatigue, mild bone pain (especially in the back or ribs), general weakness, and increased susceptibility to infections due to a compromised immune system.
Advanced symptoms include painful bone fractures occurring with little or no trauma, kidney dysfunction, severe anemia causing breathlessness and pallor, hypercalcemia (excess calcium in the blood), numbness or tingling in the hands and feet (peripheral neuropathy), unexplained weight loss, and increased thirst and urination.
CRAB Criteria
Clinicians use the CRAB acronym to identify active multiple myeloma requiring treatment:
- C — Calcium elevation (hypercalcemia)
- R — Renal impairment (kidney dysfunction)
- A — Anemia (low red blood cell count)
- B — Bone damage (lytic lesions or fractures)
If you or a loved one is experiencing any combination of these symptoms persistently, seeking prompt medical evaluation at Kannappa Memorial Hospital is strongly advised.
Causes and Risk Factors
The exact trigger that initiates the genetic mutations leading to multiple myeloma is not yet fully understood. However, research has identified several factors that increase a person’s risk:
- Age: Multiple myeloma is most commonly diagnosed at an average age of 69 and is uncommon in people under 40.
- Sex: Men are approximately 1.5 times more likely to develop multiple myeloma than women.
- Race: African ancestry is a significant risk factor people of African descent are more than twice as likely to be diagnosed compared to white populations.
- Family history:Having a close (first-degree) relative with multiple myeloma raises the risk of developing the disease.
- Obesity: Excess body weight is associated with a higher likelihood of developing the disease.
- Prior MGUS: Almost all patients with multiple myeloma have evolved from a prior stage of MGUS, even if it was undetected.
- Radiation or chemical exposure: Long-term exposure to certain industrial chemicals and radiation may increase risk.
Complications of Multiple Myeloma
When left unmanaged, multiple myeloma can cause serious and life-threatening complications:
- Bone destruction and pathological fractures result from myeloma cells triggering widespread bone breakdown. The spine is especially vulnerable, increasing the risk of spinal cord compression a medical emergency that requires immediate treatment.
- Kidney failure occurs when the abnormal M proteins deposit in the kidney tubules, impairing filtration. This is one of the most common and serious complications of active multiple myeloma.
- Severe infections are common because myeloma cells replace normal antibody-producing cells, dramatically weakening immune defenses.
- Hyperviscosity syndrome arises when excess M proteins thicken the blood, potentially causing blurred vision, headaches, and bleeding.
- Amyloidosis occurs when abnormal proteins deposit in tissues and organs, causing organ damage beyond the kidneys.
Diagnosing Multiple Myeloma
Diagnosis involves a combination of laboratory investigations, imaging studies, and tissue examination.At Kannappa Memorial Hospital, our multidisciplinary team uses the most current diagnostic criteria established by the International Myeloma Working Group (IMWG).
- Blood tests: Form the first line of investigation. A Complete Blood Count (CBC) identifies anemia or other blood cell abnormalities. Serum Protein Electrophoresis (SPEP) detects and quantifies M protein. The serum free light chain (FLC) test with a ratio ≥100 being diagnostically significant is a highly sensitive marker. Beta-2 microglobulin levels assist in staging.
- Urine tests: Including 24-hour Urine Protein Electrophoresis (UPEP) and Bence Jones protein testing, detect abnormal proteins excreted through the kidneys.
- Imaging: Plays a critical role in assessing bone damage and disease extent. Whole-body low-dose CT scans are standard for detecting lytic lesions. MRI is preferred for evaluating spinal involvement and soft tissue disease. PET-CT scanning is increasingly used to assess metabolic disease activity and treatment response.
- Bone marrow biopsy: Considered the most reliable procedure for confirming the diagnosis. A sample of bone marrow is extracted typically from the hip bone and analyzed to confirm the percentage of clonal plasma cells (≥10% confirms diagnosis) and identify chromosomal abnormalities through FISH (fluorescence in situ hybridization) testing, which directly informs prognosis and treatment planning.
Staging and Prognosis
The Revised International Staging System (R-ISS) is the globally accepted framework for staging multiple myeloma, incorporating beta-2 microglobulin, albumin levels, LDH, and cytogenetic risk:
- Stage I: Characterized by low beta-2 microglobulin levels, normal LDH values, and standard cytogenetic findings, offering the most favorable prognosis.
- Stage II: Neither Stage I nor Stage III intermediate prognosis.
- Stage III: High beta-2 microglobulin with either elevated LDH or high-risk cytogenetics most aggressive disease.
Survival estimates have improved significantly with modern therapy. Real-world data show overall survival exceeding 10 years in transplant-eligible patients treated with current regimens. Even among elderly patients over 75, median overall survival has reached approximately 5 years. Localized disease (solitary plasmacytoma) carries a 5-year survival rate of 82.1%. Importantly, these statistics continue to improve as newer therapies enter clinical practice. Patients diagnosed today should expect better outcomes than historical data suggest.
Treatment Options for Multiple Myeloma
Treatment is tailored to the patient’s stage, cytogenetic risk, age, overall health, and eligibility for transplant. Kannappa Memorial Hospital’s oncology team offers the full spectrum of evidence-based therapies.
- Watchful Waiting: Used for MGUS and low-risk smoldering myeloma, this approach involves regular monitoring with blood tests and clinical evaluations every few months, delaying therapy until signs of progression appear.
- Drug Therapy: Combination drug regimens form the backbone of treatment for active disease. These typically include proteasome inhibitors, immunomodulatory drugs, monoclonal antibodies, and corticosteroids, which work together to target and control myeloma cells.
- Stem Cell Transplant (ASCT): For eligible patients, autologous stem cell transplant uses the patient’s own stem cells after high-dose chemotherapy to achieve deeper and longer-lasting remission.
- CAR T-Cell Therapy and Advanced Treatments: For relapsed or refractory disease, CAR T-cell therapy and other novel immunotherapies offer highly targeted approaches that harness the immune system to destroy cancer cells.
- Radiation Therapy: Used for localized bone pain, spinal cord compression, or isolated tumors.
- Supportive Care: Includes bone-strengthening drugs, infection prevention, pain management, anemia treatment, and kidney protection to manage complications and improve daily functioning.
Clinical Trials and Emerging Therapies
Myeloma research is advancing rapidly.
- Bispecific antibodies such as teclistamab and elranatamab simultaneously target BCMA on myeloma cells and CD3 on T cells, showing remarkable response rates in relapsed disease.
- Precision medicine approaches leverage cytogenetic profiling to match patients with therapies most likely to be effective for their specific tumor biology.
- Minimal Residual Disease (MRD) negativity is now a key treatment goal achieving MRD negativity correlates with longer progression-free survival.
Kannappa Memorial Hospital encourages eligible patients to explore clinical trial participation, which provides access to innovative therapies while contributing to advances that will benefit future patients.
Living With Multiple Myeloma
A diagnosis of multiple myeloma requires attention not only to medical treatment but also to physical, emotional, and social wellbeing.
- Nutrition and Exercise: Adequate calcium and vitamin D intake supports bone health. Weight-bearing exercise, as tolerated, helps maintain bone density and muscle strength. A registered dietitian can help patients optimize nutrition during treatment.
- Mental and Emotional Health: Anxiety, depression, and fear of relapse are common and valid responses to a serious diagnosis. Counseling, peer support groups, and mind-body practices can meaningfully improve quality of life. At Kannappa Memorial Hospital, we provide access to psychological support and connect patients with myeloma-specific support communities.
- Ongoing Monitoring: After achieving remission, regular follow-up with blood tests, protein studies, and imaging is essential to detect relapse early when treatment can again be most effective. Managing treatment side effects such as neuropathy, fatigue, and bone pain is an ongoing part of care.
Prevention and Risk Reduction
- There is currently no proven way to prevent multiple myeloma. However, maintaining a healthy body weight, avoiding unnecessary radiation exposure, and not smoking are reasonable protective measures.
- Individuals with confirmed MGUS should maintain their recommended monitoring schedule the earlier a progression to active myeloma is detected, the greater the range of treatment options available.
When to See a Doctor
Timely medical consultation is essential if you notice any of the following symptoms
- Persistent or unexplained bone pain, particularly in the back or ribs
- Recurrent infections or infections that are slow to resolve
- Extreme and unexplained fatigue
- Fractures occurring with minimal trauma
- Numbness, tingling, or weakness in the limbs
- Unexplained weight loss or excessive thirst and urination
Early evaluation including simple blood and urine tests can detect multiple myeloma or its precursor conditions before significant organ damage occurs. At Kannappa Memorial Hospital, our hematology and oncology specialists are equipped with the diagnostic technology and clinical expertise to evaluate, diagnose, and create a personalized treatment plan for every patient.
Patient Testimonials
Dr. Gopinath at Kannappa Memorial Hospital is an exceptional hematologist. From my very first appointment, I felt like I was in incredibly capable and caring hands. He took the time to really listen to my concerns and explain my diagnosis in a way that was both informative and reassuring. What impressed me most was his genuine empathy and compassion.I’m so grateful for his expertise and the excellent care I received. I highly recommend Dr. Gopinath to anyone seeking a compassionate and skilled hematologist
Conclusion
Multiple myeloma is a complex but increasingly treatable blood cancer. Advances in quadruplet induction regimens, autologous stem cell transplantation, CAR T-cell therapy, and bispecific antibodies have transformed what was once a uniformly poor prognosis into a condition in which long-term remission and for some patients, many years of excellent quality of life is achievable.
At Kannappa Memorial Hospital, our integrated approach to multiple myeloma care combines world-class diagnostic precision, evidence-based treatment, and compassionate patient support because every patient deserves the best possible chance at a meaningful life beyond diagnosis.
Read more: Lymphoma Cancer Symptoms