Bone marrow transplant, also known as stem cell transplant, is one of the most advanced medical treatments in modern hematology. It is primarily used to treat life-threatening blood disorders such as leukemia, lymphoma, multiple myeloma, aplastic anemia, thalassemia, and certain immune deficiency conditions.
Although this procedure can be life-saving and potentially curative, it is also associated with a wide spectrum of complications. Understanding Bone Marrow Transplant Side Effects is essential for patients and caregivers because early identification and proper management significantly improve survival outcomes and quality of life.
These side effects occur due to intensive conditioning therapy (high-dose chemotherapy and sometimes radiotherapy), immune system suppression, and immune reactions from donor cells in allogeneic transplants.
Why Side Effects Occur in Bone Marrow Transplant
A bone marrow transplant replaces damaged or diseased hematopoietic stem cells with healthy stem cells. Before transplantation, patients undergo a conditioning regimen designed to destroy abnormal cells and suppress the immune system to prevent rejection.
However, this aggressive preparation leads to significant physiological stress. The main causes of Bone Marrow Transplant Side Effects include:
- High-dose chemotherapy toxicity damaging healthy tissues
- Radiation-induced injury (in some cases)
- Complete immune suppression leading to infection vulnerability
- Donor immune system attacking host tissues (GVHD)
Because of these factors, patients require intensive monitoring in specialized transplant units such as those available at Kannappa Memorial Hospital, where multidisciplinary teams manage both acute and long-term complications.
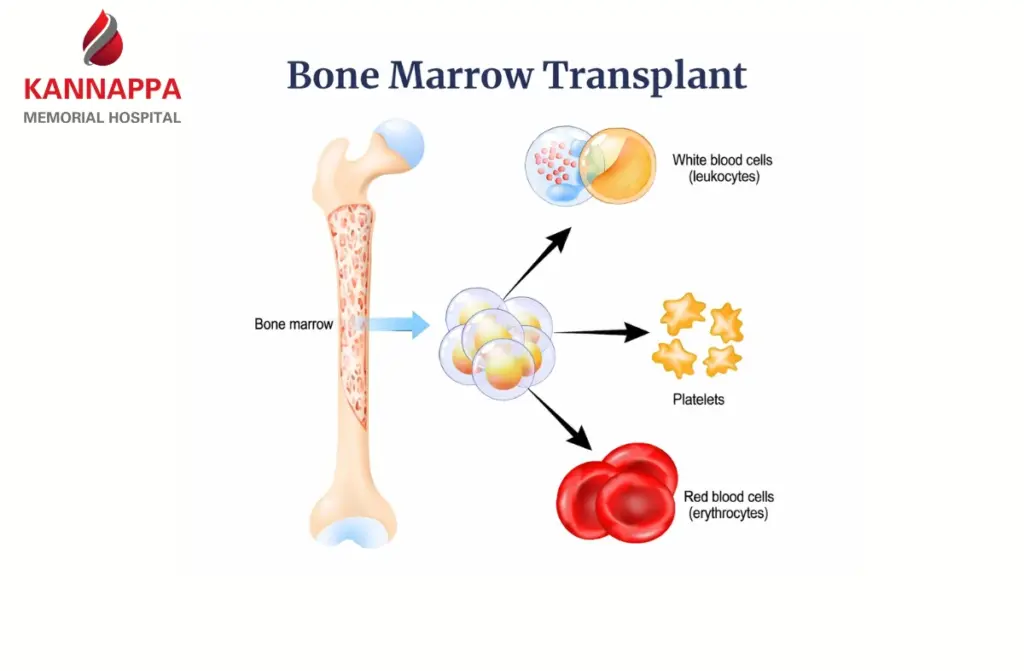
Classification of Bone Marrow Transplant Side Effects
Understanding the timeline of complications helps doctors anticipate and treat issues early.
Early Phase (Day 0 to 30 Days)
This phase includes the conditioning period and immediate post-transplant stage. Most complications are acute and severe.
Common issues:
- Severe drop in blood counts
- Infection risk due to neutropenia
- Gastrointestinal toxicity
- Mucositis and oral ulcers
- Fatigue and weakness
Intermediate Phase (1 to 3 Months)
This is the engraftment period when new stem cells begin producing blood cells.
Complications include:
- Delayed engraftment
- Early graft-versus-host disease (GVHD)
- Persistent infections
- Organ stress
Late Phase (Beyond 3 Months to Years)
Long-term survivors may develop chronic complications such as:
- Organ dysfunction
- Hormonal imbalance
- Infertility
- Secondary cancers
- Chronic GVHD
Early Bone Marrow Transplant Side Effects
Bone Marrow Suppression (Pancytopenia)
One of the most predictable Bone Marrow Transplant Side Effects is pancytopenia, where all blood cell types decrease dramatically.
Effects:
- Red blood cell reduction → severe fatigue, breathlessness
- White blood cell reduction → life-threatening infections
- Platelet reduction → A decrease in platelets can lead to bleeding gums, easy bruising, and internal bleeding.
Patients often require:
- Frequent blood transfusions
- Platelet transfusions
- Growth factor injections (e.g., G-CSF)
This phase is medically critical because even minor infections can become severe.
Infections: The Most Dangerous Early Complication
Due to immune suppression, infection remains one of the leading causes of complications.
Types of infections:
- Bacterial infections: bloodstream infections and pneumonia
- Viral infections: CMV, HSV reactivation
- Fungal infections: Candida, Aspergillus
Why risk is high:
- Neutropenia (low neutrophils)
- Damaged mucosal barriers
- Hospital exposure
Prevention:
- Sterile isolation rooms
- Prophylactic antibiotics and antifungals
- Strict hand hygiene protocols
- Regular viral monitoring
At advanced centers like Kannappa Memorial Hospital, infection control protocols are strictly followed to reduce mortality risk.
Gastrointestinal Toxicity
Chemotherapy targets rapidly dividing cells, which includes the lining of the digestive tract.
Symptoms:
- Severe nausea and vomiting
- Diarrhea
- Abdominal pain
- Loss of appetite
These symptoms often result in nutritional deficiencies, requiring IV fluids or parenteral nutrition.
Mucositis (Oral and Throat Complications)
Mucositis is one of the most painful complications of transplant.
Effects:
- Mouth ulcers
- Severe throat pain
- Difficulty swallowing
- Secondary infections
Proper oral hygiene and pain management are essential for maintaining nutrition.
Fatigue and Weakness
Fatigue is a universal symptom in transplant patients. It results from anemia, inflammation, poor nutrition, and emotional stress. Recovery may take months even after discharge.
Hair and Skin Changes
Chemotherapy affects rapidly dividing skin and hair cells.
Effects:
- Hair loss (temporary alopecia)
- Skin dryness and peeling
- Sensitivity to sunlight
- Nail changes
Hair typically regrows after treatment completion.
Major Complications of Bone Marrow Transplant
Bone marrow transplant can be life-saving, but it may also lead to serious complications that need close monitoring and treatment.
- Graft-versus-Host Disease (GVHD): GVHD is one of the most important complications in allogeneic transplants. It happens when the donor’s immune cells attack the patient’s body. It can affect the skin (rashes, itching), gut (diarrhea, stomach pain), and liver (jaundice). GVHD can be acute (within the first 100 days) or chronic (long-term condition). Treatment includes steroids, immunosuppressive medicines, and advanced biological therapies if needed.
- 4.2 Graft Failure: Sometimes the transplanted stem cells do not grow properly. This is called graft failure. It leads to very low blood counts, repeated infections, and may require another transplant or additional treatment.
- 4.3 Organ Toxicity: High-dose chemotherapy and radiation used before transplant can damage organs. This may affect the liver (SOS), lungs (pneumonitis), heart (cardiotoxicity), kidneys (renal damage), and nerves (neuropathy). Careful planning and dose control help reduce these risks.
Overall, these complications are managed with strict monitoring and specialized post-transplant care to improve patient safety and outcomes.
Intermediate Phase Complications
During engraftment, the immune system is still weak.
Common issues:
- Slow recovery of immunity: After transplant, the immune system takes time to become strong, so patients remain vulnerable to illness.
- Repeated infections: Due to weak immunity, patients may get frequent bacterial, viral, or fungal infections.
- Early signs of GVHD: Donor cells may start attacking the body, causing symptoms like skin rash, diarrhea, or liver problems.
- Tiredness and low energy: Patients often feel weak and fatigued because of treatment, anemia, and slow recovery.
- Loss of appetite: Many patients eat less due to medications, illness, or general weakness, which can affect recovery.
Long-Term Bone Marrow Transplant Side Effects
Bone marrow transplant can save lives, but it may also cause some long-term side effects that need regular monitoring.
- Organ damage: Some patients may develop long-term problems in organs such as the heart, lungs, kidneys, or liver. This can happen due to strong chemotherapy or radiation used during treatment. Regular check-ups help in early detection and management.
- Fertility issues: Fertility may be impacted in both males and females. Some patients may face infertility, hormonal changes, or early menopause in women. Doctors may suggest preserving sperm or eggs before the transplant if needed.
- Secondary cancers: There is a small risk of developing new cancers later in life, such as blood cancers like leukemia or MDS, or other solid tumors. This risk is linked to previous chemotherapy and radiation exposure.
- Hormonal and eye problems: Some patients may develop hormonal imbalances, thyroid disorders, growth-related issues, or cataracts, especially after radiation therapy.
- Relapse of disease: In some cases, the original disease may return months or years after treatment. This is more common in high-risk patients and requires long-term follow-up care.
Rare but Serious Conditions
- Post-transplant lymphoproliferative disorder (PTLD): A condition where immune cells grow abnormally after transplant due to weak immunity, often linked to EBV infection.
- EBV-associated lymphoma: A type of cancer caused by Epstein-Barr virus in immunosuppressed patients after transplant.
- Severe sepsis: A life-threatening condition caused by a severe body response to infection, leading to organ dysfunction.
- Multi-organ failure: Failure of more than one organ (like kidneys, liver, lungs) due to severe illness, infection, or complications after transplant.
Psychological and Emotional Effects
The emotional burden of transplant recovery is significant.
Common issues:
- Anxiety: Patients may feel constant worry about treatment, recovery, and future health.
- Depression: Feelings of sadness, low mood, and loss of interest are common after serious illness or long treatment.
- Fear of relapse: Patients often worry that the disease may return even after successful treatment.
- Social withdrawal: Patients may avoid social interactions due to weakness, emotional stress, or fear of infection.
Psychological counseling and family involvement are essential parts of recovery.
Monitoring and Management of Side Effects
Proper post-transplant care improves survival significantly.
Key strategies:
- 1. Regular blood tests and imaging: Blood tests are done regularly to check blood counts, organ function, and detect early complications. Imaging may be used to monitor disease status.
- 2. Infection surveillance: Patients are closely monitored for infections because their immunity is weak. Early detection and treatment are important.
- 3. Immunosuppressive therapy: Medicines are given to prevent rejection and reduce graft-versus-host disease (GVHD), especially in allogeneic transplant.
- 4. Nutritional support: Proper diet is important for recovery, healing, and maintaining immunity. Supplements may be given if needed.
- 5. Pain management: Pain is controlled using medications to improve comfort and recovery.
- 6. Long-term follow-up clinics: Regular follow-up is needed to monitor late complications, relapse, and overall health after transplant.
At specialized centers like Kannappa Memorial Hospital, structured transplant follow-up programs help patients manage both physical and emotional recovery effectively.
Recovery and Prognosis
Recovery after transplant is gradual:
- Engraftment: 2–4 weeks
- Immune recovery: 6 months to 2 years
- Full recovery: varies by patient
Factors affecting outcome of transplantation
1. Age
Younger patients usually have better outcomes. Older patients have more complications and slower recovery.
2. Underlying disease
Outcome depends on the disease type and stage. Patients in early stage or remission do better than those with advanced disease.
3. Type of transplant
- Autologous transplant: lower complications, but higher chance of relapse.
- Allogeneic transplant: higher risk of complications but better disease control in some cancers.
- Better donor match improves results.
4. Complications
- GVHD (Graft-versus-host disease): donor cells attack the body, mainly in allogeneic transplant.
- Infections: common due to weak immunity after transplant and can be severe.
Early rehabilitation improves outcomes significantly.
Conclusion
Bone Marrow Transplant Side Effects occur across early, intermediate, and long-term stages, ranging from mild to serious complications. Early effects include infections, low blood counts, and treatment-related toxicity, while intermediate and late stages may involve graft-versus-host disease (GVHD), delayed immune recovery, and organ damage. Major risks such as infections, GVHD, and organ toxicity require prompt medical attention to ensure better outcomes.
Long-term issues may include infertility, hormonal imbalance, and secondary cancers, making regular follow-up essential. Emotional and psychological health also plays a key role in recovery. With modern advances, improved monitoring, and expert multidisciplinary care such as at Kannappa Memorial Hospital patients now have significantly better survival and long-term quality of life.