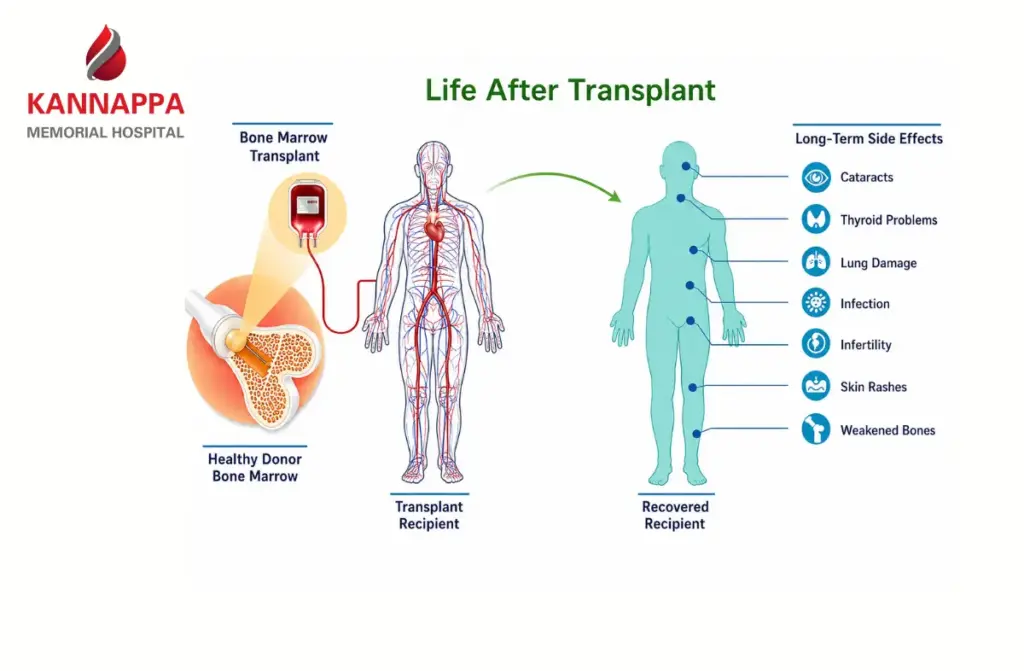
A Bone Marrow Transplant (BMT) is one of the most advanced medical procedures used to treat life-threatening blood and immune system disorders. It replaces damaged or diseased bone marrow with healthy stem cells, helping the body restore its ability to produce healthy blood cells. For many patients, this procedure is not just a treatment it’s a life-saving intervention that offers a second chance at life.
Over the years, Chennai has emerged as a leading destination for advanced medical care in India. The city combines world-class expertise, experienced transplant specialists, and significantly lower treatment costs. Hospitals like Kannappa Memorial Hospital play an important role in delivering advanced transplant care with a patient-focused approach. The Bone Marrow Transplant Cost in Chennai typically ranges from ₹10,00,000 to ₹40,00,000+, depending on medical complexity and treatment needs.
Cost of Bone Marrow Transplant in Chennai
The Bone Marrow Transplant Cost in Chennai is one of the most important deciding factors for families planning this highly specialized and life-saving treatment. Since BMT involves multiple stages of intensive care, advanced diagnostics, and long-term follow-up, the overall expense can vary widely depending on the patient’s condition and medical requirements.
Chennai has earned a strong reputation in India’s healthcare system for offering advanced transplant care at comparatively affordable prices, while maintaining global standards of treatment quality, safety, and clinical outcomes.
Estimated Cost Range
The total cost of bone marrow transplant in Chennai generally falls within the following range:
- Minimum Cost: ₹10,00,000
- Average Cost: ₹18,00,000 – ₹25,00,000
- Maximum Cost: ₹40,00,000+
This estimate typically includes pre-transplant evaluation, hospital stay in isolation units, transplant procedure, medications, ICU support (if required), and initial post-transplant recovery monitoring.
It is important to understand that this is not a fixed package cost. Instead, it is a clinical cost range, which changes based on individual medical needs.
Cost Breakdown & Key Factors
a. Cost Components
Understanding the breakdown helps patients plan finances better:
- Tests & Diagnostics: Blood tests, imaging, and compatibility testing
- Hospital Stay: Includes isolation rooms and specialized care units
- Doctor Fees: Hematologists, transplant specialists, and support staff
- ICU & Medications: Intensive care support and the use of specialized, high-cost medications.
- Post-Transplant Care: Follow-ups, medications, and monitoring
Each of these contributes to the overall Bone Marrow Transplant Cost in Chennai.
b. Factors Affecting Cost
Several variables influence the final cost:
- Type of Transplant: Autologous is usually cheaper than allogeneic
- Donor Match Complexity: Perfect matches reduce complications and cost
- Patient’s Condition: Advanced disease may require longer care
- Hospital Choice: Premium facilities may charge higher
- Complications: Infections or graft rejection can increase expenses
What is Bone Marrow Transplant?
A Bone Marrow Transplant (BMT) is a treatment procedure that replaces damaged or diseased bone marrow with healthy stem cells. Bone marrow is the soft, spongy tissue inside bones that produces blood cells—red cells, white cells, and platelets which are essential for carrying oxygen, fighting infections, and preventing bleeding.
When the bone marrow is not functioning properly due to disease, infection, or intensive cancer treatment, a transplant helps restore normal blood cell production.
Types of Bone Marrow Transplant
Bone marrow transplantation can be classified into several types based on the source of stem cells. Each type is chosen according to the patient’s medical condition, disease severity, and donor availability. The goal of all transplant types is to restore healthy blood cell production and improve immune system function.
- Autologous Transplant: Uses the patient’s own stem cells, collected and stored before undergoing high-dose chemotherapy or radiation. This type reduces the risk of rejection and graft-versus-host disease, making it a safer option for certain cancers like lymphoma and multiple myeloma.
- Allogeneic Transplant: Uses stem cells donated by another person, usually a fully matched sibling or an unrelated donor. This type is commonly used for blood cancers and genetic disorders, as the donor cells can also help attack remaining cancer cells through a graft-versus-leukemia effect.
- Haploidentical Transplant: Uses stem cells from a partially matched donor, often a close family member such as a parent or child. It increases the chances of finding a suitable donor quickly and has become more widely used due to advances in transplant techniques and infection control.
- Cord Blood Transplant: Uses stem cells collected from the umbilical cord blood of a newborn baby and stored in cord blood banks. These cells are more flexible in matching requirements and are especially useful for pediatric patients or those without a suitable donor.
Diseases Treated by Bone Marrow Transplant (BMT)
A Bone Marrow Transplant (BMT) is used to treat a wide range of serious conditions affecting the blood, bone marrow, and immune system. It works by replacing damaged or diseased marrow with healthy stem cells, helping the body produce normal blood cells.
Cancers
BMT is commonly used to treat blood-related cancers, such as:
- Leukemia: A cancer of the blood and bone marrow that affects white blood cells.
- Lymphoma: Cancer of the lymphatic system, including Hodgkin and non-Hodgkin lymphoma.
- Multiple myeloma – A type of cancer that affects plasma cells in the bone marrow.
Blood Disorders
BMT helps restore healthy blood cell production in severe conditions like:
- Thalassemia: A genetic disorder causing abnormal hemoglobin formation.
- Aplastic Anemia: A condition where the bone marrow fails to produce enough red blood cells, white blood cells, and platelets.
Genetic & Immune System Disorders
BMT can correct certain inherited and immune deficiencies by replacing faulty cells:
- Severe Combined Immunodeficiency (SCID): A rare disorder where the immune system is extremely weak.
- Sickle Cell Disease: A genetic blood disorder affecting red blood cell shape and function.
- Other Disorders: Includes certain metabolic and inherited immune system conditions.
Bone Marrow Transplant offers a potential cure or long-term control for many of these diseases, especially when other treatments are not effective.
When is a BMT Needed?
Doctors may recommend a Bone Marrow Transplant (BMT) when underlying bone marrow or blood disorders severely affect normal body functions or do not respond to standard treatments.
Common Indications:
- Frequent or Severe Infections: A weakened immune system makes the body more vulnerable to recurring infections
- Persistent Fatigue and Weakness: Caused by low levels of healthy blood cells
- Abnormal Blood Counts: Irregular levels of red cells, white cells, or platelets detected in tests
- Failure of Conventional Treatments: When medications or other therapies do not produce effective results
These signs often point to serious bone marrow dysfunction, where a transplant may be necessary to restore healthy blood cell production and improve overall health outcomes.
Pre-Transplant Preparation
Preparation is a very important phase in Bone Marrow Transplant (BMT), as it ensures the patient is physically and mentally ready for the procedure. Proper evaluation helps reduce risks, identify complications early, and improve overall success rates.
Key Preparation Steps:
- Comprehensive Tests & Scans: A series of detailed blood tests, bone marrow tests, and imaging scans are done to understand the patient’s current health condition and disease status. These tests help doctors plan the most suitable transplant approach.
- Organ Function Assessment: The functioning of major organs such as the heart, liver, kidneys, and lungs is carefully evaluated. This ensures that the patient can safely tolerate high-dose chemotherapy or radiation used during the transplant process.
- HLA Matching: Human Leukocyte Antigen (HLA) typing is performed to find the best possible donor match. A closer match reduces the risk of complications like graft rejection and graft-versus-host disease (GVHD), improving transplant success.
- Patient Counseling: Patients and their families receive psychological and emotional counseling to prepare them for the treatment journey. This includes understanding possible risks, recovery time, lifestyle changes, and post-transplant care.
Thorough pre-transplant preparation is essential for minimizing risks, ensuring proper planning, and significantly increasing the chances of a successful Bone Marrow Transplant outcome.
Procedure
The Bone Marrow Transplant (BMT) process is carried out in a carefully planned sequence to ensure safety, effectiveness, and better recovery outcomes.
Step-by-Step Process:
- Conditioning Therapy: High-dose chemotherapy and/or radiation is given to eliminate diseased cells, suppress the immune system, and create space in the bone marrow for new stem cells.
- Stem Cell Collection: Healthy stem cells are collected either from the patient (autologous transplant) or from a matched donor (allogeneic transplant), depending on the treatment plan.
- Infusion: The collected stem cells are infused into the patient’s bloodstream through an intravenous line, similar to a blood transfusion, and the procedure is usually painless.
- Engraftment: The infused stem cells travel to the bone marrow, settle, and begin producing new red blood cells, white blood cells, and platelets over the next few weeks.
This entire process is performed in specialized transplant units under strict medical supervision, with continuous monitoring to manage side effects and ensure proper recovery.
Risks & Complications
Like any major medical procedure, Bone Marrow Transplant (BMT) carries certain risks and possible complications. However, with advanced treatment methods and close monitoring, many of these can be managed effectively.
Common Risks:
- Infections: After transplant, the immune system becomes weak, making patients more prone to bacterial, viral, and fungal infections. Strict hygiene and protective care are essential during recovery.
- Bleeding Issues: Low platelet counts can lead to easy bruising, gum bleeding, or internal bleeding, requiring regular monitoring and transfusions if needed.
- Organ Damage: High-dose chemotherapy or radiation may temporarily or permanently affect organs such as the liver, lungs, heart, or kidneys.
- Graft Failure: In some cases, the transplanted stem cells may fail to grow or function properly, requiring additional treatment or a repeat transplant.
- Disease Relapse: There is a chance that the original disease may return after some time, depending on the condition being treated and patient response.
With early detection, preventive care, and expert medical supervision, these risks can be significantly reduced, improving the overall success of Bone Marrow Transplantation.
Benefits & Success Rate
Bone Marrow Transplant (BMT) offers meaningful advantages for patients with severe blood and immune system disorders. Although it is a complex and intensive procedure, it can be life-changing when performed under appropriate medical conditions.
Benefits:
- Provides the possibility of a complete cure or long-term remission
- Improves overall survival rates across various conditions
- Enhances quality of life by restoring the body’s ability to produce healthy blood cells
Success Rate:
The success rate of BMT typically ranges from 50% to 80%, depending on several important factors, including:
- The type of disease being treated
- The stage and severity of the condition
- The level of compatibility between donor and recipient
With continuous advancements in medical technology, transplantation techniques, and supportive care, success rates are steadily improving—making BMT an increasingly effective and promising treatment option for eligible patients.
Recovery & Aftercare
Recovery after a Bone Marrow Transplant (BMT) is a slow and carefully monitored process that requires patience, discipline, and regular medical follow-up.
Key Aspects of Recovery:
- Long-Term Monitoring: Patients need frequent follow-up visits, blood tests, and check-ups to monitor recovery, detect complications early, and ensure proper functioning of the new stem cells.
- Medications: Doctors prescribe immunosuppressive drugs and other supportive medications to prevent infections, control side effects, and reduce the risk of graft-versus-host disease (GVHD).
- Strict Hygiene: Maintaining proper hygiene is very important, as the immune system remains weak for some time. This includes clean surroundings, safe food habits, and infection prevention practices.
- Recovery Timeline: Recovery varies from patient to patient and may take several months to a year or more, depending on overall health, transplant type, and response to treatment.
Following medical advice carefully and maintaining regular care plays a major role in ensuring a smooth recovery and long-term success after BMT.
Conclusion
A Bone Marrow Transplant (BMT) is a complex yet life-saving procedure for patients with severe blood disorders, cancers, and immune conditions. It involves multiple stages such as diagnosis, donor matching, treatment, and long-term recovery, but can greatly improve survival and quality of life.
Chennai has become a leading hub for advanced transplant care, offering expert doctors, modern facilities, and affordable treatment. The Bone Marrow Transplant Cost in Chennai typically ranges from ₹10,00,000 to ₹40,00,000+, making it cost-effective compared to many countries. With advancing technology, outcomes are improving, and hospitals like Kannappa Memorial Hospital support patient-focused, structured transplant care.
Read Also: Best Anemia Doctors in Chennai